Pandemics… the great leveler?
Sociologist Fabrizio Bernardi discusses how socio-economic status figures in as a risk factor for COVID-19.
Author:


Reading time: 6 min.
Pandemics are seen as a leveler…but are they? While detailed data on the socio-economic status of COVID-19 victims are still not available, much indirect evidence suggests that the risk of falling seriously ill and dying from COVID-19 is higher among individuals with lower incomes and lower levels of education.
Early data indicate that income could matter
There is now evidence showing a higher risk of mortality for some ethnic minorities in the UK and among African-Americans in the United States, populations also disproportionately in the lower quintiles of income and educational distributions. Aggregate data indicate higher COVID-19 mortality in the poorest neighborhoods of the USA and départements in France.
What people risk
COVID-19 mortality risk can be conceived as the result of the product of three different risks: the risk of infection, the risk of developing a severe disease from coronavirus and the risk of dying/recovering if severely ill with COVID-19. In the below sections, I will discuss how low educational and economic status might be related to each of these risks.
Risk of infection
First, with regard to the risk of infection we can assume that at the beginning of the pandemic, most people had an equal probability of catching the virus. It has actually been said that this coronavirus travelled in business class. The so called ‘patient zero’ in Italy is a manager, and one of the first coronavirus hotspots in Europe was a ski resort in Austria. However, the situation changed for people under lockdown and during the partial resumption of economic activity. Many low-skilled workers in professions with high risk of infection due to high proximity to others, such as cashiers, couriers and workers in the energy sector and construction, never stopped working. In phase two, while smart working from home remains an option for managers, scientists and high-level professionals, it is not a possibility for low-level factory workers or those working in service jobs.
Risk of developing severe disease with COVID-19
We know that people with underlying pre-existing medical conditions are more vulnerable to becoming severely ill with COVID-19. We also know that the incidence of chronic diseases among elderly people tends to be higher among those who are low-educated. Figure 1 shows the incidence of at least one chronic disease among those older than 64 in Italy, broken down by education level. Similar results hold for other EU countries. Among the low educated about one in two (48%) suffers fromat least one chronic disease, compared to one in three (31%) among those with a university degree. Among men the educational gradient is slightly less steep but still pronounced. Incidentally, the higher incidence of chronic disease among men than among women is also likely to explain their higher mortality by COVID-19.
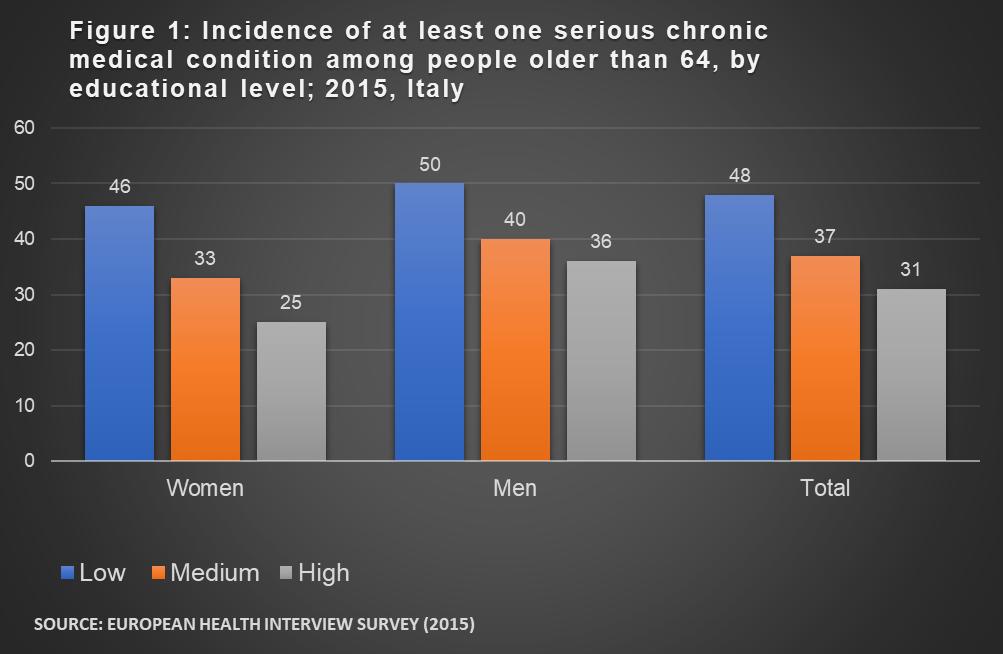
Why are lower-educated people more at risk for pre-existing conditions? They are more likely to have poor health lifestyles, they often do physically taxing work, they are more exposed to stress and they tend to have worse access to medical care and prevention.
Risk of dying from COVID-19
Pulling through from a serious COVID-19 infection depends to a large extent on the probability of receiving adequate medical treatment, for instance having timely access to an intensive care unit. For the moment we can assume that in EU countries there are no significant economic differences in access to adequate medical treatment, but that is probably not the case in the US and other systems which lack good or affordable national health systems.
A note on nursing homes
There is one last point related to COVID-19 inequalities, and this regards nursing homes and other care facilities. The available evidence suggests that nursing homes are a critical trouble spot in the COVID-19 pandemic. According to a recent report published with the International Long-Term Care Policy Network, in Belgium and France about half of the deaths linked to COVID-19 happened in nursing homes. Similar or higher proportions are reported in Italy and documented by the media in Sweden, the Netherlands, and Spain.
For people in nursing homes, the highest values for the three risks related to the COVID-19 discussed above, i.e. the risks of infection, of developing a serious form of disease and of not receiving adequate treatment, converge. Nursing home residents share common spaces, and have daily contact with caring aides who move from patient to patient, which increases the risk that the disease might spread. They usually have pre-existing health conditions that make them more vulnerable and, in case of illness, the quality of medical treatment in nursing homes is generally inferior to hospital treatment.
Who is likely to live in a nursing home? In a recent paper I wrote with Marco Cozzani and Francesca Zanasi, we used SHARE data on 13 EU countries to analyse how the probability of living in nursing and care homes varies by the respondent’s level of education. Our results show that in all countries included in the study, individuals with low education are more likely to live in nursing homes, with odds ratios equal or greater than two in many cases . Given the extremely high death toll in care homes, evidence on differences in the probability of being in a care home also provides indirect but clear evidence of the existence of social inequality in the risk of mortality linked to COVID-19.
Lower educated populations probably are at greater risk for COVID-19
It seems, then, very plausible that the lowest educated are those most severely affected by the coronavirus. They are more likely to work outside home in jobs posing higher risks of infection. They are more likely to have pre-existing health conditions that make them more vulnerable to developing severe forms of the disease. They are also more likely to live in a nursing and care homes, where the highest mortality rates are observed.
These conclusions fly in the face of assertions that the new coronavirus affects everyone equally. It also raises questions of social justice. In these dramatic days we all have felt defenseless towards COVID-19, but it is clear that some people—and not just health workers—are more exposed and vulnerable than others.
The COVID-19 pandemic provides yet another reason why reducing social inequality should be a priority, now more than ever.
Professor Fabrizio Bernardi is Professor of Sociology in the Department of Political and Social Sciences. He is the elected Chair of the Board of the European Consortium for Social Research, and a founding member and co-Director of the Comparative Life Course and Inequality Research Centre at the EUI.